Ablation Surgery May Be More Effective Than Drugs For A-Fib
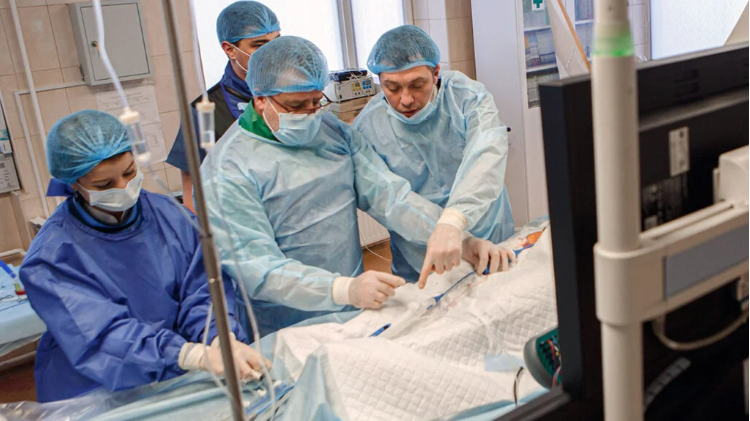
A recent randomized clinical trial showed that the use of cryoballoon ablation, a type of catheter ablation, as an initial treatment was associated with lower rates of progression of atrial fibrillation than antiarrhythmic drugs.
Studies suggest that around 1 to 2% of individuals in the United States have atrial fibrillation (A-fib). A-fib can become more severe over time, progressing from short episodes to more persistent forms characterized by longer and more frequent episodes. Studies suggest that persistent A-Fib is associated with an increased risk of stroke, heart failure, and mortality.
A recent study published in The New England Journal of Medicineshows that cryoballoon ablation was associated with a lower rate of progression from short episodes to persistent A-fib.
In an interview with Medical News Today, the study’s author Dr. Jason Andrade, a cardiac electrophysiologist at Vancouver General Hospital, said:
“Until now, we did not have any intervention proven to modify the progression of the disease. In contrast to medications, we see that ablation is able to modify the pathophysiology of the disease. This was a finding that was observed despite selecting a population at low objective risk of progression.
“This finding built on our previous work, which demonstrated that first-line ablation led to less short-term recurrence, a lower burden of AF [A-fib], higher likelihood of symptom resolution, greater improvement in quality of life, and lower subsequent healthcare utilization.”
Atrial fibrillation (A-fib): Things to know
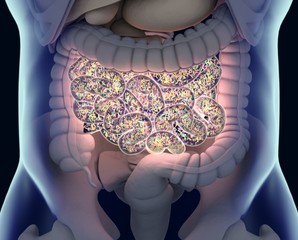
The heart has four chambers- two upper chambers called the atria, and two lower chambers called the ventricles. The atria and ventricles contract alternately to pump blood to the body during each cardiac cycle.
The sinoatrial node or sinus node, a cluster of muscle cells located in the right atrium, helps maintain a normal heart rhythm and acts as the natural pacemaker. The sinus node generates electrical impulses that travel through a pathway of specialized muscle cells in the atria and the ventricles.
As the electrical impulses travel through the atria and down to the ventricles, these impulses cause the sequential contraction of these chambers. This results in the pumping of blood from the atria to the ventricles and then from the ventricles to the body. The rhythmic firing of the cells in the sinus node helps maintain a normal resting heart rate of 60 to 100 beats per minute in healthy individuals.
The disruption of these electrical impulses leads to an abnormal rate or rhythm of a person’s heartbeat, known as arrhythmia. A-fib, one of the most common forms of arrhythmia, is characterized by the contraction of the atria in a disorganized fashion.
In A-fib, the heart receives electrical impulses from sources other than the sinoatrial node. The resulting disordered electrical impulses lead to the rapid and chaotic contraction or quivering (fibrillation) of the atria.
The irregular heart rhythms in A-fib can lead to the formation of blood clots in the atria, which can travel and obstruct blood vessels, causing a stroke or embolism. In addition, patients with A-fib are at increased risk of heart failure and cardiovascular mortality.
A-fib is a progressive condition, with episodes becoming more frequent and longer with time. The condition can be classified according to the duration of an episode.
Paroxysmal A-fib refers to episodes that spontaneously stop within seven days. On the other hand, episodes that last longer than seven days are known as persistent atrial fibrillation. In long-standing persistent A-fib, episodes occur uninterrupted for more than 12 months.
The authors of the present study note that an estimated 8 to 15% of individuals with paroxysmal A-fib cases tend to develop persistent A-fib within the first 12 months. Moreover, individuals with persistent A-fib are at a greater risk of heart failure and thromboembolism, the obstruction of blood vessels due to a blood clot.